No products in the cart.
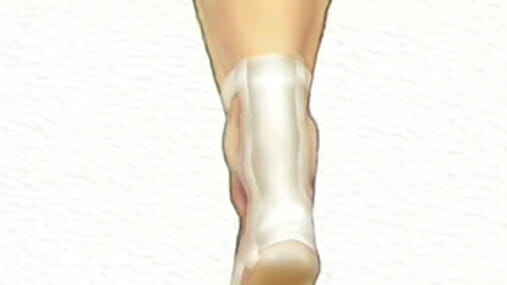
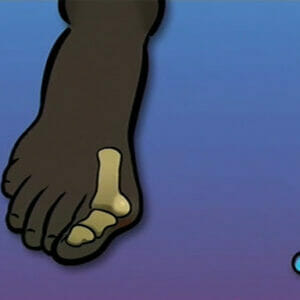
Achilles Tendon Repair Surgery
$299.00 — or $99.00 / year
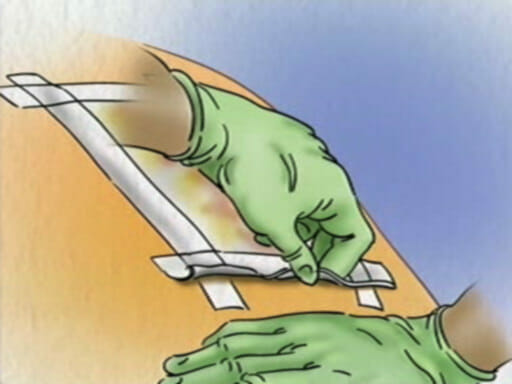
This animated medical illustrated video: Achilles Tendon Repair Surgery describes the Achilles tendon and explains the surgery to repair a rupture.
You may also like…
-

Achilles Tendon Repair Surgery
$299.00 — or $99.00 / year Add to cart -

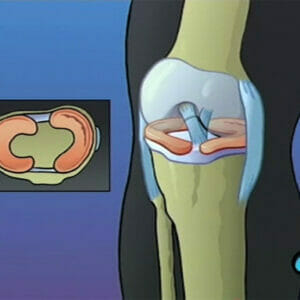
Anterior Cruciate Ligament (ACL) Arthroscopic Repair Surgery
$299.00 — or $99.00 / year Add to cart -

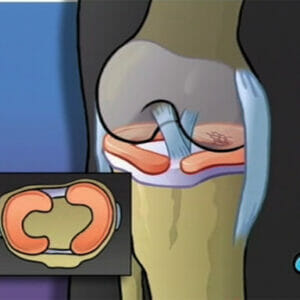
Arthroscopic Meniscus Repair of Knee
$299.00 — or $99.00 / year Add to cart -

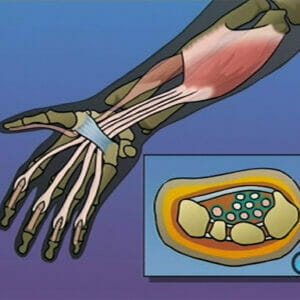
Carpal Tunnel Syndrome Repair Surgery
$299.00 — or $99.00 / year Add to cart -

Hip Replacement Surgery
$299.00 — or $99.00 / year Add to cart -

Knee Replacement Surgery
$299.00 — or $99.00 / year Add to cart -

Rotator Cuff Repair – Arthroscopic
$299.00 — or $99.00 / year Add to cart -

Rotator Cuff Repair Open
$299.00 — or $99.00 / year Add to cart -

Shoulder Replacement
$299.00 — or $99.00 / year Add to cart